Know when it’s a clinical indicator or wake up call
Standard in every skilled nursing therapist’s day is dealing with patients’ refusal of therapy. A typical SNF therapist averages 1-2 refusals of treatment each day. That can be 15-20 percent of a therapist’s day that’s canceled!
Of all those therapy refusals, most are legitimate. But among them, there are some SNF patients who could be motivated to get up and exercise.
Often, a motivated therapist can cajole a patient to join the scheduled therapy session. But many times, it’s simply easier for a busy therapist to let a tired or distracted patient skip a session.
And now with PDPM, where SNFs are no longer reimbursed for therapy minutes, therapists have even less motivation to counter patients’ refusals than they once did under the RUG-IV payment plan with CMS.
However, therapy is the key reason patients enter a skilled nursing rehab center, and its centrality to patient care is unquestionably essential. Skilled nursing therapy is key to the healing process and to slowing the physical and mental decline of aging patients.
PDPM means therapists and SNFs are focused more on quality than quantity, but that still means that a patient who is prescribed any number of weekly therapy sessions absolutely needs to access those sessions in order to achieve the best outcome.
The responsibility lies on the therapist to make sure refusals don’t stand in the way of accessing therapy.
3 underlying reasons skilled nursing patients refuse therapy
Patients will have a whole host of reasons for refusing therapy, and most of them are absolutely legitimate. It’s up to you as a therapist to consider how the patient is responding and determine the source of the refusal. This way, you can determine if the reason is something you can work around or if it’s a sign of a bigger issue. And sometimes, refusals just might mean that you have work to do to make therapy sessions more worthwhile.
Reason #1: Patient isn’t feeling well
Patients may be adjusting to a new medication, still healing from a recent procedure or have any number of clinical challenges that can make therapy more difficult. Speak to interdisciplinary team members to see if they have also received concerns and what subsequent actions have been taken
Reason #2: Patient has concerns outside of their control
Skilled nursing care has to be integrative for therapists to successfully treat patients. This means letting the care team know when a patient doesn’t get enough sleep because of a loud roommate or a patient didn’t eat because the food got too cold. Be an advocate for the patient if action has not been taken to address concerns/complaints.
Reason #3: Patient is apathetic
Sometimes patients will refuse therapy without a specific reason. Statements like “Maybe tomorrow?” or “I don’t want to do it today” can mean that the patient isn’t seeing the value of the therapy sessions.
Reassess your approach to skilled nursing therapy for apathetic patients
If you are unable to identify the source of why your patient is refusing care, it’s time to ask yourself some hard questions.
We as therapists are taught the therapeutic use of self approach. This means we use all our faculties to meet our patients where they are, with empathy, and bring them to where we want them to be for the session. We use our creativity, attitude, and effort to make patients feel positive, motivated, encouraged, and successful. This is how we gain their trust and ensure they feel empowered.
7 questions therapists should ask when facing refusals
- Are you offering a care approach that has meaning to the patient?
- Are you offering a care approach in which the patient believes they have the opportunity to experience success?
- Can you grade your approach to gain trust and agreement?
- Are you conveying enthusiasm and excitement in your approach or are you going through the motions and thinking about the end of the day?
- What is your strategy to motivate?
- Can you modify the environment to one that will promote a more successful experience?
- Can you modify the intended activity based on the fluctuating physical and cognitive ability output of your patient?
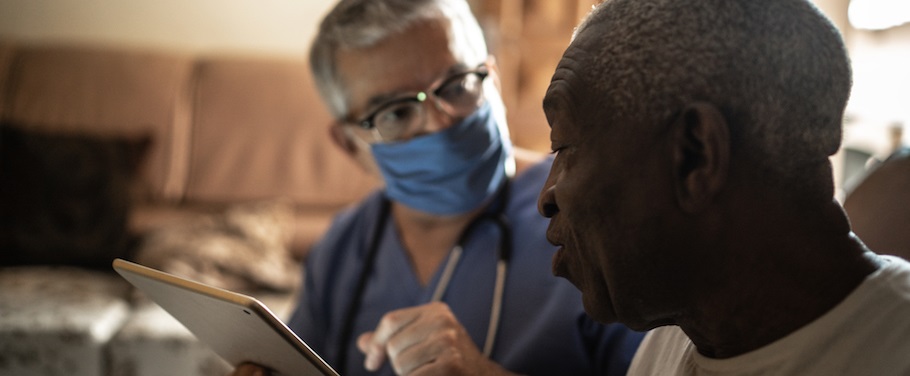
Therapists’ methods to deal with refusals
Once you’ve taken some time to ask yourself the hard questions above, you are poised to better address therapy refusals. The following are some steps you can use.
Step 1: Show empathy to patients’ needs
Your first reaction to therapy refusals should always be empathy. Most patients have legitimate hesitations to therapy, such as overall weakness, pain or emotional struggles. Of course, therapy can improve the physical and mental state of patients, but it’s a long process, and the journey can be hard.
Listen well to your patients’ concerns and repeat what you hear them saying to you to validate their concerns. If the patient is refusing to exercise because he is in pain or needs an improvement to his care, you may need to advocate for him to the interdisciplinary team.
Step 2: Use a person-centered approach for therapy
One obvious solution to refusals, of course, is to have a more person-centered approach. Provide therapy on the patients’ schedule, when he is at his best. This is obviously harder to coordinate, but if it reduces refusals to offer a late sleeper a later therapy time slot, then you will have more luck cajoling him to exercise.
It also helps to offer the patient something engaging she wants to do. Get to know her interests and goals and relate the therapy back to those goals. Your patient wants to walk her granddaughter down the aisle? Remind her that it starts with working on standing for two minutes.
Don’t be afraid to get family members involved in what a patient enjoys. Therapy is a great time to jump on a Zoom call with a patient’s loved ones. This makes the family feel connected, increases transparency, motivates the patient and helps you get to know more about the patient. This is why we included a video-conferencing tool right within our RESTORE Skills therapy gaming platform.
Step 3: Make therapy fun and engaging
Armed with the latest technology that makes therapy interactive, engaging and even fun, therapists can significantly reduce refusals. As the Chief Clinical Officer of RESTORE Skills, where we’ve created just this kind of therapy gaming platform, I see examples every day of patients actually requesting to play our therapy games. They are motivated by the fun they are having skiing, golfing or playing the slot machines, as well as the results they see as they improve their game scores.
To add to the joy, we are known for an “I hit the jackpot with RESTORE” t-shirt for those patients who hit “Wild, Wild, Wild” on our slot machine game. We are constantly hearing about patients relentlessly playing this therapy game until they win. Meanwhile, they are actually winning at therapy, as they push themselves to reach and stretch farther.
The right attitude, approach, and activity can make therapy easier and reduce refusals, but sometimes you need added help
Refusals can feel personal. Most therapists have developed conscious and subconscious defense mechanisms related to these remarks. However, simply shielding yourself from the impact is not necessarily best for your patient or your professional growth and development.
Even the most passionate and creative therapists will still face regular refusals on the job. This is where innovative technology can fill the gap. Having access to a variety of interactive treatment content and the ability to connect loved ones for added encouragement and participation is the perfect compliment to an empathetic, positive and motivating therapist’s approach. Hope these strategies help you realize better outcomes with less refusals.